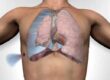
This is a gland that rests behind the breast bone (also called the sternum). It is different from the thyroid gland which lies in the neck. The thymus is associated with the immune system and helps fight infection and disease. It is active until puberty and then shrinks away so that only fatty tissue remains in adulthood. After puberty, the thymus does not play an important role, and removing it does not result in any ill effects or any problems with the immune system.
Myasthenia gravis (MG) is an autoimmune disorder caused, in most cases, by autoantibodies against components of the neuromuscular junction, frequently the acetylcholine receptor (AChR), and less often the muscle-specific kinase receptor. The thymus plays a major role in the pathogenesis of MG with anti-AChR antibodies.
- For younger MG patients the thymus gland is often swollen (referred to as hyperplasia).
- 10% of MG patients (1 out of 10 patients) may have a tumor of the thymus gland, which is called a thymoma.
- Symptoms of MG may include droopy eyelids; blurred or double vision; difficulty speaking, swallowing, and breathing; and muscle weakness.
Why do I Need a Thymectomy?
Based on the results of the international clinical trial, it is now recommended that people with MG who have acetylcholine receptor antibodies in their blood are referred for thymectomy.

There are two different types of thymectomy:
1. Video-Assisted Thoracoscopic Surgery (VATS)
VATS stands for Video-Assisted Thoracoscopic Surgery, where the thymus gland is removed via keyhole surgery. Recovery from this surgery is quick and you are usually in hospital for 1-3 days.
2. Trans-sternal Thymectomy
This is a more extensive procedure where the surgeon makes a cut on the chest wall, the sternum (breast bone) is split and they remove the thymus through this cut. Recovery from this surgery is longer and you may need to stay in hospital for 4-6 days.
Long-lasting benefit
The researchers found that the benefit from thymectomy continues to be seen up to five years after the procedure with improvement continuing to exceed that seen with medical therapy alone.
Patients who had the surgery and continued to take prednisone were able to take significantly lower doses of the steroid than patients who didn’t have the surgery.
The need for hospitalizations, such as intensive care admissions to treat MG exacerbations, is reduced by some two-thirds compared to medical therapy alone.
- In about 60% of patients, thymectomy results in significant improvement in the patient’s muscle weakness.
- In some cases (about 30%) thymectomy results in permanent remission (meaning you no longer need medication).
- However, in some patients, thymectomy makes no difference to their myasthenia.
What are the risks of a Thymectomy?
- Sometimes the surgeon finds at surgery that it is technically difficult to remove the thymus gland by VATS or RATS, and you may need to have a trans-sternal thymectomy instead. The surgeon will be able to convert to a trans-sternal thymectomy during the same procedure (on the same day).
- Bleeding.
- Pain and discomfort.
- Phrenic nerve palsy (damage to the nerves which run in the chest)
When can I return to my usual activities?
This will depend on your muscle weakness, the type of procedure you have had and the type of activities you do. Please discuss this with your consultant.
After trans-sternal thymectomy you can return to driving after 6 weeks. After keyhole surgery (VATS or RATS), you will be able to drive after 2 weeks.
You will be able to fly 6 weeks after either procedure.
Follow-up
You will have a follow-up appointment with the surgeon, usually around 6 weeks after the surgery. The myasthenia team will also arrange to see you soon after your surgery in case changes are needed to be made to your medications.
Conclusion
Thymectomy can be an option even in elderly patients, provided the operation is performed early after the onset.
References
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6351377/#
https://www.myaware.org/thymectomy-information-sheet
https://www.technologynetworks.com/neuroscience/news/thymus-removal-benefits-myasthenia-gravis-patients-for-up-to-five-years-after-surgery-314555