What Causes Body Odor and How Can I Treat It?
What is bromhidrosis?
Bromhidrosis is foul-smelling body odor related to your sweat.
Perspiration itself actually has no odor. It’s only when sweat encounters bacteria on the skin that a smell can emerge. Other than body odor (BO), bromhidrosis is also known by other clinical terms, including osmidrosis and bromidrosis.
Bromhidrosis can often be treated or prevented through changes to your hygiene habits, though there are medical treatment options as well.
Introduction
Sweat-related body odor manifests in essentially all individuals at some point during life. Excessively foul-smelling sweat is considered pathologic and termed bromhidrosis, a term derived from the Greek “bromos” (stench) and “hidros” (sweat). Synonyms of bromhidrosis include “bromidrosis,” “osmidrosis,” and “ozochrotia.”
The degree of odor considered “excessive” and sufficient for a diagnosis of bromhidrosis is not definitive. Bromhidrosis is generally diagnosed when noticeable body odor has a negative effect on an individual’s self-view, social interactions, or quality of life.
Bromhidrosis is divided into apocrine bromhidrosis and eccrine bromhidrosis. The most common site for apocrine bromhidrosis is the axilla. Eccrine bromhidrosis most often affects the feet.
The clinical features, diagnosis, and management of bromhidrosis will be reviewed here. Hyperhidrosis (excessive sweating) is reviewed separately.
Subtypes
Bromhidrosis is subdivided into apocrine and eccrine variants based upon the type of sweat gland involved. Apocrine glands develop after puberty and are most densely distributed in the axillae, anogenital areas, and breasts. The primary role of apocrine glands appears to be the secretion of pheromones. Eccrine glands are widely distributed all over the body, with the exception of the external auditory canal, lips, clitoris, labia minora, and glans penis. Eccrine glands are primarily responsible for thermoregulation.
Symptoms
Some people naturally sweat more or less than other people. Body odor also can vary from person to person. See a doctor if:
- You suddenly begin to sweat much more or less than usual
- Sweating disrupts your daily routine
- You experience night sweats for no apparent reason
- You notice a change in your body odor

Causes
Sweating and body odor are caused by sweat glands in your body. The two main types of sweat glands are eccrine glands and apocrine glands. Eccrine glands occur over most of your body and open directly onto the surface of the skin. When your body temperature rises, these glands release fluids that cool your body as they evaporate.
Apocrine glands are found in areas where you have hair, such as your armpits and groin. These glands release a milky fluid when you’re stressed. This fluid is odorless until it combines with bacteria on your skin.
Treatment
The appropriate treatment approaches for bromhidrosis are based on the severity of the condition. In some cases, preventive measures are enough. In more serious cases, removal of the offending sweat glands may be the answer. Your treatment options include:
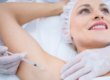
Botox
Botulinum toxin A (Botox), which works by blocking nerve impulses to the muscles, can be injected into the underarm to block nerve impulses to the sweat glands. The downside of Botox treatment is that it wears off after a while, so you may need it a few times a year. Botox is also used for sweaty hands and feet.
Surgical removal of apocrine glands is a valid treatment option for axillary bromhidrosis. However, malodor may recur after the operation. The value of botulinum toxin A (BTX-A) injection in the treatment of secondary axillary bromhidrosis was investigated in the present study. From July of 2012 to May 2016, 53 patients with secondary axillary bromhidrosis were enrolled in our clinic. Various BTX-A injection strategies were applied depending on different types of previous surgery. None of the patients reported adverse side effects after the procedure. The duration of efficacy ranged from 1 to 12 months, with a median value of 6 months. At the end of follow-up, 48 patients ranked the satisfaction with BTX-A treatment as “very good” or “good”. For patients with secondary axillary bromhidrosis following various surgical modalities, the BTX-A treatment strategy we propose can achieve a longer duration of efficacy with a low risk of side effects and should be considered a good and reliable option.
Liposuction (LC)
One way to cut down on apocrine sweat is to remove the sweat glands themselves. You may have heard about liposuction in relation to removing fat from your midsection or elsewhere in the body. Special tubes are carefully inserted into the body, and fat is extracted.
The same concept can be applied to sweat glands under your arms. A very small suction tube, called a cannula, is inserted just under the skin. It’s then grazed along the underside of your skin, removing sweat glands as it goes. This process may leave some glands in place that can continue to cause excessive sweating.
A meta-analysis showed that the curative effect of LC was equivalent to the other 2 methods but that the complication rate in LC was less than those in laser treatment and open excision. The results of this meta-analysis suggest that LC, which has fewer complications, can be considered as the primary choice in the treatment of patients with bromhidrosis compared with other surgical procedures.
Surgery
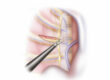
A more invasive way of removing sweat glands or the nerves that trigger sweating is through surgery. A procedure called endoscopic sympathectomy uses small incisions and special tools to clip or cut or cauterize (burn) the sympathetic nerves in the chest that lead to the underarm sweat glands. The procedure is effective for more than 12 years.
Another minimally invasive treatment is called electrosurgery. It’s done with tiny insulated needles. Over a period of several treatments, a doctor can use the needles to remove the sweat glands.
Surgery is more preferable and commonly used for serious cases. However, postoperative complications and the formation of scars remain the problems with surgical treatment. Conventional surgery entails 1 or 2 longitudinal incisions in the axillary area, and the use of ophthalmic scissors to destroy subcutaneous apocrine sweat glands to achieve the targeted therapeutic outcomes.
The addition of drainage holes can effectively drain off subcutaneous exudate and reduce the degree of swelling. However, based on our experience, 0.3 cm-long drainage holes cannot completely eliminate congestion or exudate production. Therefore, we extended the length of the drainage holes to 0.5 cm and averaged them in the same design as the Sudoku puzzle. At the same time, we used anchors to secure the skin to the subcutaneous tissue. This method has been shown to enable adequate drainage and good fixation, which can effectively reduce the occurrence of subcutaneous hematoma, and leave less obvious scars.
In conclusion, our improved surgical procedure to treat bromhidrosis can effectively eliminate underarm odor and has a low risk of complications. This significantly improves patient quality of life postoperatively compared to that with the traditional procedure.
Home remedies
Before any invasive procedure is attempted, you should try some basic hygiene strategies. These can help reduce the number of bacteria interacting with your sweat. These life hacks for beating BO are a great place to start.
Because bromhidrosis is triggered by the action of bacteria on the skin, frequent washing may be enough to neutralize the bacteria. Washing at least daily with soap and water may help. If the smell is localized to the armpits, for example, you can focus your cleansing efforts there.
An antiseptic soap and antibacterial creams containing erythromycin and clindamycin may also help.
A strong deodorant or antiperspirant can play a key role in minimizing odor. Trimming the hair in your underarms is also recommended.
You should also wash your clothes regularly and remove clothes that are sweaty as soon as you can. While some clothes can be worn more than once before washing as a general rule, if you have bromhidrosis, you may need to wash after every wear. An undershirt may help keep the odor from reaching your outer layers of clothing.
References
- J Plast Reconstr Aesthet Surg. 2017 Nov;70(11):1641-1645
- Medicine (Baltimore). 2017 Aug; 96(33): e7844
- Medicine (Baltimore). 2019 May; 98(22): e15865
- https://www.healthline.com/health/bromhidrosis#treatment
- https://www.mayoclinic.org/diseases-conditions/sweating-and-body-odor/symptoms-causes/syc-20353895
- https://www.uptodate.com/contents/bromhidrosis#:~:text=Bromhidrosis%20is%20generally%20diagnosed%20when,apocrine%20bromhidrosis%20is%20the%20axilla.